De Quervain’s Tenosynovitis
WHAT IS DE QUERVAIN’S TENOSYNOVITIS?
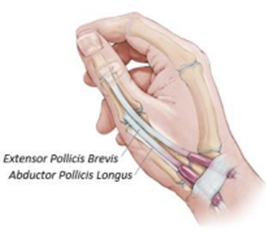
De Quervain’s tenosynovitis occurs when the tendons around the base of the thumb are irritated, inflamed or constricted. Changes of the tendon sheath that covers two of the tendons responsible for moving the thumb can cause pain and tenderness along the thumb side of the wrist. This often occurs when lifting the thumb, forming a fist, grasping, gripping things or when turning the wrist.
SYMPTOMS
- Pain along the thumb side of the forearm, near the wrist.
- Difficulty and pain moving your thumb and wrist when doing activities that involve grasping or pinching.
- Weakness in the hand.
- A “sticking” or “stop-and-go” sensation in your thumb when trying to move it.
DIAGNOSIS
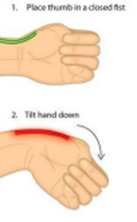
De Quervain’s Tenosynovitis can be detected by making a fist then moving the wrist down in the direction of the little finger.
It is also assessed by bending at the wrist and resisting the thumb moving towards the forearm.
These tests are usually quite painful compared to the unaffected hand/wrist. There may also be local tenderness with palpation/pressure directly over the tendon.
Diagnosis can also be confirmed with an ultrasound which can detect if there is any local inflammation.
TREATMENT
Conservative Management
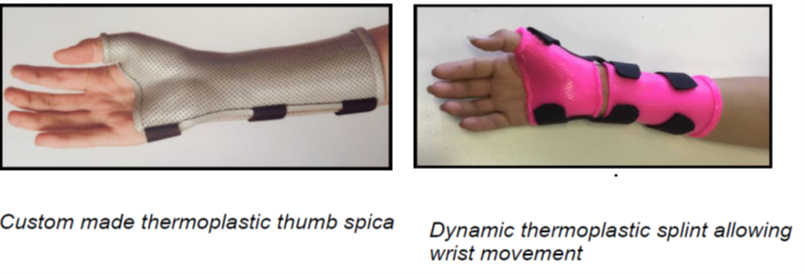
- Splints – worn for 3-6 weeks or until settled with aggravating or at risk activities. They provide rest and immobilisation of the inflamed tendons of the thumb. These splints can be hard and custom made by your therapist (thermoplastic thumb spica) or semi-rigid (neoprene + thermoplastic).
- Heat/ice
- Anti-inflammatory medication
- Ultrasound
- Wrist stretches
- Advice on returning to work (eg. taking frequent rest breaks during repetitive tasks, keeping wrist in neutral alignment when possible).
- Adapting manual repetitive work activities which aggravate the pain.
- Addressing postural issues and muscle imbalances.
- Progression to a strengthening program once pain and inflammation is reduced
Cortisone Injection
- Strong evidence supports those with moderate to severe pain benefiting from cortisone injection and splinting
Surgical Management
- Surgery is rare and is usually recommended if symptoms do not subside and continue to affect function after at least 6 weeks of conservative management and cortisone injection.
- The goal of surgery is to release the tendons and give them more space, so they no longer rub on the inside of the tunnel.
- Therapy is also beneficial post surgery to optimise normal functional use of the hand, restore full range of motion and to increase strength.